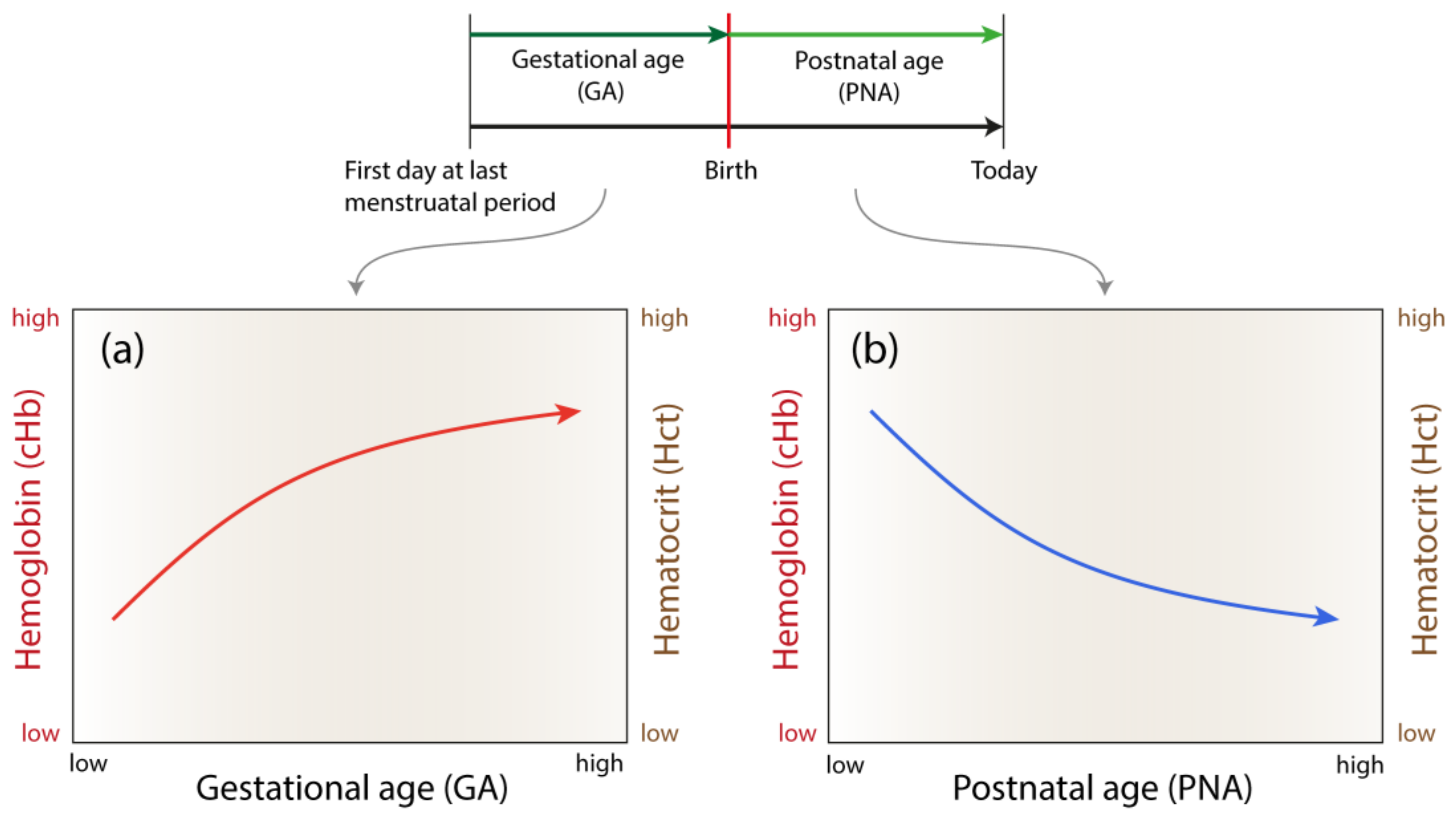
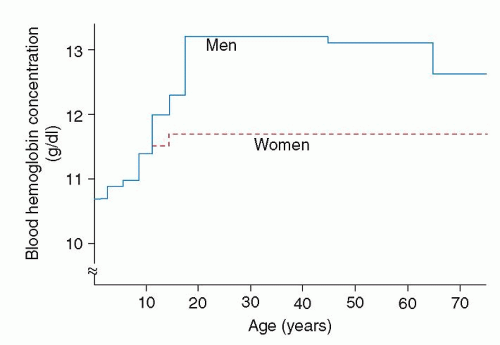
Therefore, it is essential to clarify the meaning of the report results from the respective medical professional. Usually, a 7% difference (in higher or lower values) is seen among different diagnostic centers. Note that the values may vary from one medical authority to another. The normal range in men is 40 to 54%, while for women the values range between 36 to 48%. The hematocrit is reported as a percentage of the volume of red blood cells in 100 ml of blood. The normal acceptable level of hemoglobin in men and women ranges between 14 to 18 g/dl and 12 to 16 g/dl respectively g/dl being the abbreviation for the measuring unit ‘grams per deciliter’. The values of both these components can be determined by conducting a complete blood count (CBC) test, as both are based on plasma volume. On the other hand, hematocrit is the measurement of the amount of RBCs present in the total blood volume. Hemoglobin (Hb) is the protein found in RBCs that carries oxygen to the entire body. There are about one billion red blood cells in two to three drops of blood, and for every 600 red blood cells, there are about 40 platelets and one white cell.īoth hemoglobin and hematocrit are linked with red blood cells (RBCs). This HealthHearty article gives you an overview of the symptoms and possible causes that could trigger the same. Talk with the healthcare provider about how your baby is likely to progress.Low hematocrit and hemoglobin levels signify a decrease in red blood cells (RBCs) in the body.
Once treated, anemia does not cause long-term complications for most babies. This treatment is not routinely used and may have side effects. The medicine prompts the baby’s body to make more red blood cells. Medicine may be given to the baby through an IV line or by injection. The donor blood helps bring the baby’s red blood cell count back to normal. This is done through an IV (intravenous) line. Talk with the healthcare provider about the cause of your baby’s hemolysis.Ī blood transfusion puts healthy donor blood into the baby’s body. As a result, the baby’s red blood cells don’t live as long. These antibodies are now in the baby’s blood. During pregnancy, the mother’s body made substances called antibodies that fought against the baby’s red blood cells. Also in some newborns, the baby’s blood type is incompatible with the mother’s blood type. Newborn red blood cells don't live as long as adults' red blood cells do. Shortened red blood cell life (hemolysis). This means the baby’s red blood cells aren’t living as long as they’re supposed to. When a baby is born early, less iron is stored and the body is less able to respond to the need to make more red blood cells. Normally, the baby’s body stores iron during the last months of pregnancy. Low red blood cell production. This occurs if the baby doesn’t get enough iron (a nutrient that helps build red blood cells). Blood loss can also occur in twins if one twin got less blood than the other during pregnancy (called a twin-to-twin transfusion). This is called a fetal-maternal transfusion. In some cases, some of the baby’s blood moves into the mother’s bloodstream during pregnancy. A baby who has a hemorrhage (internal bleeding) could also become anemic.

Because of this risk, NICUs try to limit the amount of blood drawn as much as possible. This is because blood must be taken from the baby so certain tests can be done. Your baby’s anemia is likely caused by at least one of these problems:īlood loss. This is a common cause of anemia in babies in the NICU (neonatal intensive care unit). It must be treated to bring the red blood cell count back up. Many babies have mild anemia within a few months after birth. As a result, the baby feels tired and has less energy. When a baby has anemia, the body doesn’t get enough oxygen. Red blood cells carry oxygen throughout the body.

This means the baby’s blood contains fewer red blood cells than normal. Your newborn has been diagnosed with anemia.
